Research Centre for Brain and Behaviour
Research with the human experience at its heart
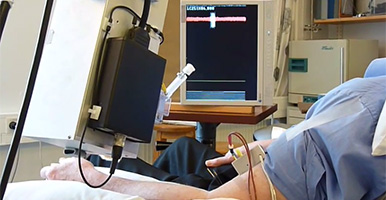
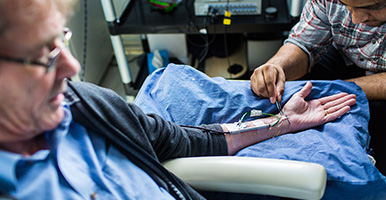
Our centre is home to many research approaches that aim to understand the psychology of human experience and – broadly speaking – investigate how we experience, feel, think, and behave. We employ a large variety of research methodologies, including many neuroscientific tools to study the role of the brain in these processes.
We use a whole toolbox of psychological methods – quantitative and qualitative alike – to drill deep into the emotions, motivations, cognitions, and habits that influence and govern our behaviours. We focus on mental and physical health and wellbeing, on various factors that play a role in preserving health and factors that can be enlisted to promote and enhance health and wellbeing. Our research covers the whole human lifespan, starting even before birth and covering the ageing process.
Our People:
In total, more than 60 colleagues are involved in this research, and we support more than 50 postgraduate research students. Find out more within each research theme.
Our Research Excellence:
The latest national assessment of research excellence (the REF2021) confirmed the high quality of research carried out under the roof of our research centre. Most research we do was submitted under the Unit of Assessment 4: Psychology, Psychiatry and Neuroscience.
Around 44% of our research was rated as internationally excellent or world leading and we saw a significant increase in our research power, a measure of the overall strength of our research. We are now ranked in 37th place (of 93) regarding research power, a jump of 31 places since the REF2014.
From all post-92 institutions our submission was the 4th largest for this Unit of Assessment and we are ranked 8th out of 45 institutions. From the nine submissions in our geographical area our research is ranked 4th strongest.
Our Research Expertise
Our research is structured along four broad research themes. Take an in-depth look at our areas of expertise: