Prescription drugs pregabalin and gabapentin have been reclassified – but it won’t stop problem use

Gabapentin and pregabalin, two widely used prescription drugs, are now subject to increased controls in the UK, which means they are now reclassified as class C controlled substances.
These drugs are licensed to treat epilepsy, anxiety, peripheral and neuropathic pain (pain caused by damage or injury to the nerves), but they are known to produce feelings of euphoria, calmness and relaxation. It is this mixed profile of effects that has contributed to their wide use. But these drugs can also have serious side effects, especially when combined with other drugs – and have been associated with use of illicit street drugs.
Under the new classification, prescribers can no longer issue electronic prescriptions – they will have to be handwritten. It is also now illegal to possess these drugs without a prescription, and it is illegal to supply or sell the drugs to others.
The Advisory Council on the Misuse of Drugs (ACMD), the government’s independent scientific advisers, alerted the Home Office to a growing illicit market and the potential harms these drugs were causing. A 2016 ACMD report into these type of drugs highlighted that prescriptions for pregabalin had increased by 350% in the preceding five years and by 150% for gabapentin.
Although not as popular as other illicit drugs, there were particular concerns about their use in prisons, where there was a high number of prescriptions, as well in some parts of the UK such as Northern Ireland. Accompanying this was an alarming rise in deaths associated with their use.
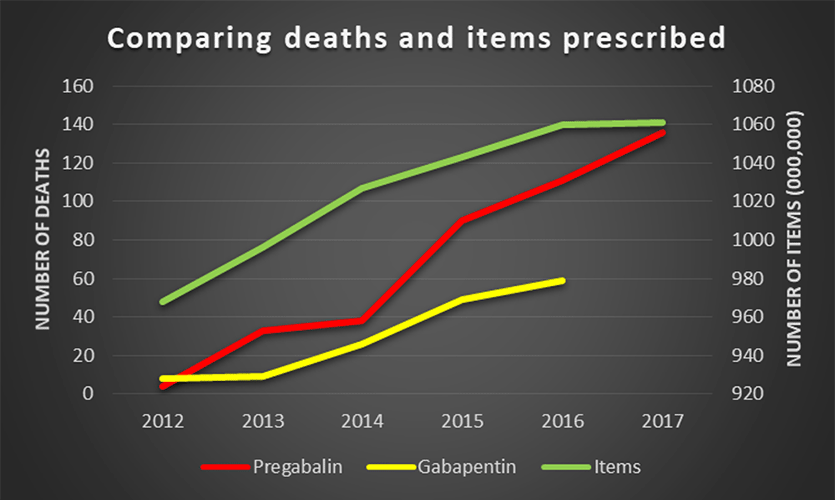
Gabapentin and pregabalin deaths compared to prescriptions.
One reason these drugs are particularly harmful is through the practice of combining them with other drugs to amplify the desired effects. For example, using gabapentin and pregabalin with heroin can increase their euphoric effects. Unfortunately, this also increases the risk of harm, as the combination has an can create breathing difficulties and reverse the tolerance that the body may have built up against heroin’s effects on breathing. This increases the risk of respiratory failure, which underpins many heroin overdose deaths.
The potential misuse of gabapentin and pregabalin has been known about for some time, but the challenge has been how to respond and reduce harm. This is not the first prescribed medication to be reclassified in this way. Tramadol, a synthetic opiate, was made a class C drug in 2014. The circumstances leading up to this change were very similar to the concerns relating to gabapentin, namely an increase in prescriptions, which was accompanied by a rise in fatalities.
Since the reclassification of tramadol, deaths have fallen as have the number of prescriptions. By this measure, it would appear that the reclassification decision for tramadol was a success. Unfortunately, it’s not that straightforward.
Shifting use
Banning or restricting the supply of drugs, whether they are legal or illegal, can produce unintended consequences. One of these is displacement, where tightening up access to one substance shifts use onto another.
It is possible that this has happened with tramadol given the rise in use of gabapentin and pregabalin – as it became harder for people to obtain, they found gabapentin and pregabalin easier to get hold of, so they became desirable alternatives. This suggests that the new restrictions on gabapentin may move the problem onto another drug, although it is likely that it will be the same group of higher risk people who are most affected. The problem is we don’t know which drug that will be, and we are unlikely to find out until the same prescribing and mortality data provide fresh information.
When we are assessing the impact of changes to drug laws, we shouldn’t solely focus on what happens to the harms associated with the drug that is banned but whether the total burden of harm from all drugs has been affected. Data showing a very high level of drug-related deaths and hospitalisations suggests that we are failing to make much of an impact.
Most people who use these drugs know the risks they face, so thinking we can simply educate or arrest our way out of this problem is unlikely to be successful. People are often attracted to using these drugs to alleviate a range of problems beyond the physical, they are often trying to mitigate psychological pain and social problems.
Accessing support for such issues has become increasingly difficult. Treatment services have faced budget cuts that restrict their ability to respond quickly. Little surprise then that people turn to drugs that have no waiting lists, can be accessed 24 hours a day and where dealers don’t ask intrusive questions.


